





















Teaching: COVID-19 Style
Faculty members adapt to COVID-19 way of teaching
There was a time when faculty members spent most of their days preparing their lectures, presenting them to their students and being available during office hours for extra instruction.



Some also had the additional task of preparing for laboratory work or work outside
of campus, such as hospitals and nursing homes. Then came the coronavirus, COVID-19,
and a new way of teaching was born.
With the return of students to Western Carolina University, and other campuses across
the country this fall, institutions had to adapt to a hybrid form of teaching, one
that includes in-person instruction with physical distancing, online instruction,
and laboratory work with smaller groups, which means offering more labs.


It also includes the wearing of face coverings – in some instances face shields –
and gloves, the usage of hand sanitizer and wiping down work areas. It has presented
a host of new challenges, but instructors have faced those challenges head on.
“I’m super busy with prep for my studio classes, which are split in half so I need
to do double the demonstrations and create individual setups for all the students
to minimize contact with shared tools and materials,” said Matt Liddle, professor in the School of Art and Design. “Also, I am doing a lot of extra cleanup after each group and reconfiguring the
space for the next class, which requires different materials. I am offering all classes
in the largest and best ventilated studio space. We are doing OK.”

Liddle has found himself using email more often to combat the challenges of keeping
his students informed and on track with their work.
Liddle has split his three classes into six different groups. In addition, he has
a small upper level class that meets concurrently with one of the groups, and a graduate
student who is working independently. And there is the matter of his 18 office hours.



To go along with the challenges COVID-19 has presented to teaching, there also are
concerns Liddle has.
“Both my family and I have health histories that put us at various levels of risk,”
he said. “In terms of teaching, I am delivering less content and missing more collaborative
work and hands-on engagement. Everything is slowed down and more complicated.”

“The students have been great, I think everybody is working really hard to stay healthy..."
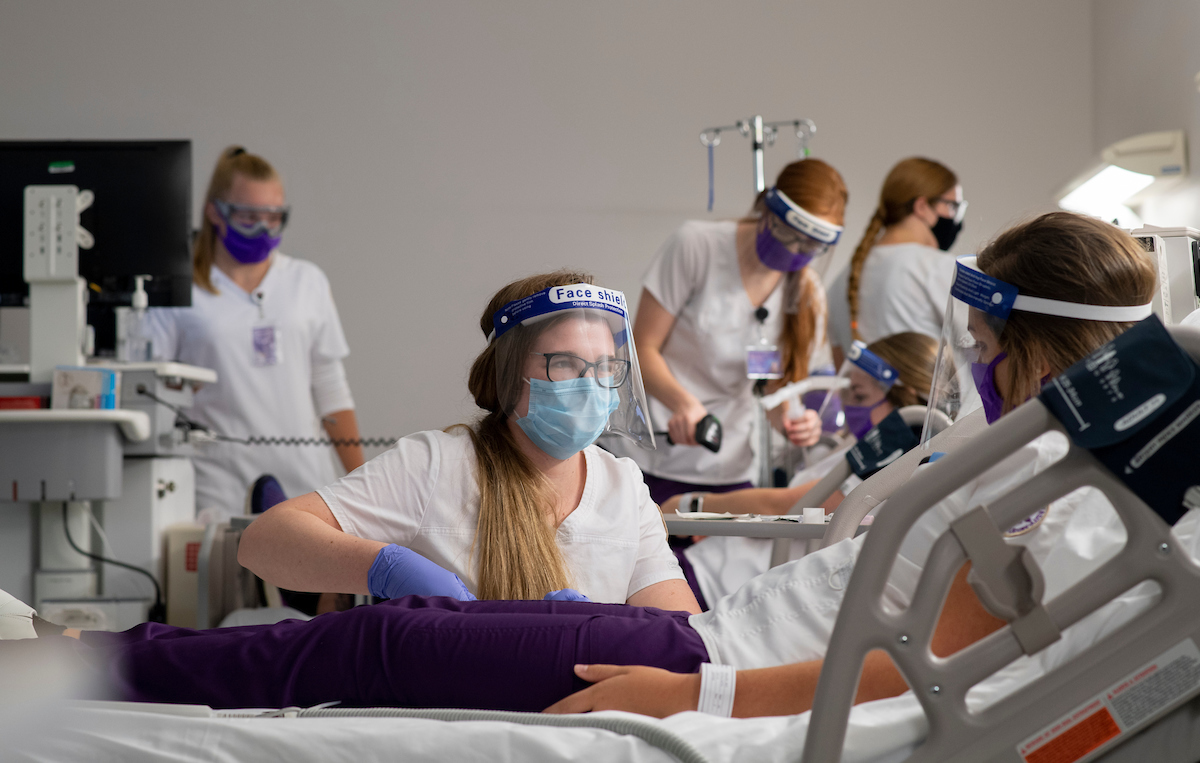
David Wells, assistant professor in the School of Nursing, primarily teaches in a simulation lab where students enact real-life nursing scenarios.
Because his labs in the past consisted of about 10 students, that part of his job
has not changed.
But Wells has been forced to hold simulation labs more frequently. Because of clinical
restrictions in the community, the scenarios in the sim labs are now longer.


“We’re having fewer clinical sites available to us, like ICU,” Wells said. “When we
lose a clinical site, we have to make those up in the simulation lab. That hasn’t
been too tough. What we found out, though, is that once we started running simulations
here, we cannot socially distance as nicely as we would like. Nurses have to touch
patients. They have to work together as a team sometimes.”
To combat that issue, the students acting as nurses and patients are wearing face
shields on top of their face masks.

“We’re into the realization that we have to get students ready for real life. Real
life in the COVID world is there’s going to be additional PPE (personal protective
equipment). There’s going to be some violation of personal space. We have to be cognizant
of that and they understand.”
During one of the simulations, students previously passed out food trays and looked
at their nutritional status. That exercise has been halted, Wells said, because the
fake food contained five to 10 pieces of fomite as possible sources of transmission.


And instead of transporting patients down the hall, up the elevator and back to the
room, they now just go to the door of the lab and turnaround.
Students acting as patients previously took off their shoes, climbed into bed and
even received a warm blanket if they wanted one. Now, all of the top linen has been
removed and students sit on the top sheet, Wells said.

“After every scenario, they have to change the top sheet, the pillowcase and the fitted
sheets, Wells said. “We do a complete linen change between patients now. … We do wipe
downs. I think we’re doing everything according to CDC guidelines. When we leave,
housekeeping comes in and they do a terminal wipe down and they mop the floors. I
think between all of us, we’re keeping it pretty clean.”
Colleen Hayes, assistant professor in the School of Nursing, has faced similar challenges in her
skills labs. She typically had 30 students in her lab at a time but has had to reduce
that number to around 10, causing her to hold three labs instead of one.



Like Wells, her students are required to wear a face mask and face shield because
it isn’t always possible to maintain six feet of physical distancing.
Hayes also utilizes the video conferencing platform, Zoom, for group discussions,
which at times is difficult.
“It’s hard to get everybody to talk and engage that way,” she said. “I do have a couple
of faculty who do labs with me, so we split some of them. We’ve cut them back from
a three-hour lab to a two-hour lab, and then give them extra prep work to do to make
up for that day. But it’s still like six hours a day when we have labs. Six hours
a day working in a mask has been an adjustment.”



The biggest positive, though, is that after a spring semester that saw professors
and students having to switch to online teaching only, everyone is glad to be back
in the classroom, regardless of the adjustments that have been made.
“The students have been great,” Hayes said. “I think everybody is working really hard
to stay healthy. They really want to go to clinical and are happy to be in clinical
and lab. It made them appreciate it more when it got taken away.”


